Crs Lin
Crs Lin
Uploaded by
PoolerErCopyright:
Available Formats
Crs Lin
Crs Lin
Uploaded by
PoolerErOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Crs Lin
Crs Lin
Uploaded by
PoolerErCopyright:
Available Formats
Downloaded from http://bjo.bmj.com/ on November 26, 2014 - Published by group.bmj.
com
Clinical science
Collagen crosslinking in the management of
advanced non-resolving microbial keratitis
Rohit Shetty, Harsha Nagaraja, Chaitra Jayadev, Yathish Shivanna, Thungappa Kugar
Narayana Nethralaya Eye
Hospital, Bangalore,
Karnataka, India
Correspondence to
Dr Harsha Nagaraja, Narayana
Nethralaya Eye Hospital, 121/
C, Chord Road, 1 R Block,
Rajajinagar, Bangalore 560
010, Karnataka, India;
harshdr@gmail.com
Received 16 January 2014
Revised 24 February 2014
Accepted 16 March 2014
Published Online First
7 April 2014
ABSTRACT
Aim To evaluate the efcacy and safety of corneal
collagen crosslinking (CXL) in the management of culture
proven microbial keratitis.
Methods 15 eyes of 15 patients of microbial keratitis
were included in the study. Nine patients had bacterial
keratitis and six had fungal keratitis. All patients
underwent microbiological evaluation to identify the
causative organism. The depth of the inltrate was
determined clinically with slit lamp and measured
manually using anterior segment optical coherence
tomography. Patients were treated with antibiotics/
antifungals and those who did not respond to at least
2 weeks of topical medications underwent CXL as per
the standard protocol. The same preoperative topical
medications were continued post-CXL. All patients were
followed up every third day and observed for signs of
resolution of microbial keratitis.
Results Six of nine patients with bacterial keratitis and
three of six patients with fungal keratitis resolved
following CXL treatment. Patients with deep stromal
keratitis or endothelial plaque failed to resolve. All
patients had resolution of pain on the rst postoperative
day. There was an appearance of or increase in
hypopyon in seven patients. No intraoperative or
postoperative complications were noticed.
Conclusions CXL appears to be an effective procedure
in the management of supercial microbial keratitis. It
can be used as an adjunctive treatment in the
management of non-resolving microbial keratitis.
INTRODUCTION
To cite: Shetty R,
Nagaraja H, Jayadev C,
et al. Br J Ophthalmol
2014;98:10331035.
Corneal diseases are a major cause of vision loss
and blindness according to WHO; ocular trauma
and corneal ulceration result in 1.52 million new
cases of corneal blindness annually.1 Microbial keratitis is characterised by a corneal epithelial defect
with underlying stromal inammation caused by
replicating microorganisms. Microbial keratitis is a
leading cause of ocular morbidity and blindness
worldwide.2 Microbial keratitis requires aggressive
management to halt the disease process and reduce
the extent of corneal scarring, which leads to loss
of vision.3 4
It has been estimated that about 50% of the eyes
have poor visual outcome if the diagnosis and
initiation of appropriate antimicrobial treatment
are delayed.5 Long-term and intensive topical
chemotherapy has led to the emergence of
multidrug-resistant bacteria that might further complicate treatment. Microbes develop resistance to
antibiotics as a result of chromosomal mutation,
inductive expression of latent chromosomal genes,
exchange of genetic material via transformation,
bacteriophage transduction or plasmid conjugation.6
The high cost of drugs, high frequency of resistance
to antibiotics, and risk of corneal melting and
corneal scars make the choice of new approaches
very desirable. Since 2000, riboavin has been used
as a photosensitiser to inactivate pathogens in
plasma, platelet and red cell products.7 8 In vitro
experiments have proven the bactericidal effect
using a 365 nm ultraviolet-A (UV-A) light photo
activation of riboavin.9 10 Multiple studies have
indicated that this could be a new tool in the management of infectious keratitis resistant to antibiotic
treatment.11 In our study, we evaluated the role of
corneal collagen crosslinking (CXL) in the management of advanced non-resolving microbial keratitis.
MATERIALS AND METHODS
Patients with non-resolving microbial keratitis were
included in the study after taking informed
consent. The study was performed under the
Tenets of the Declaration of Helsinki. At initial
presentation, all patients underwent corneal scrapping for Grams stain, potassium hydroxide preparation (KOH wet mount), bacterial culture (blood
agar and chocolate agar) and fungal culture
(Sabouraud dextrose agar). Patients were started on
topical antibiotics/topical antifungals based on the
Grams stain/KOH wet mount reports which were
obtained immediately after the patient presented to
us. There was no delay in starting topical medications in any of the patients. All patients were prescribed topical atropine 1% eye ointment in
addition to antibacterials and antifungals. They
were followed up every third day and observed for
signs of resolution of the corneal involvement and
hypopyon. Those patients not responding to
topical chemotherapy for more than 2 weeks were
considered as having non-resolving microbial keratitis involvement and advised to undergo CXL.
Patients with culture proven bacterial and fungal
keratitis were included in the study. Those patients
with perforated corneal ulcer, endophthalmitis,
viral keratitis and pregnancy were excluded.
Procedure: Topical anaesthesia was administered
using 0.5% proparacaine drops. Epithelium was not
removed as there was already a large epithelial defect
overlying the area of keratitis in all patients.
Riboavin drops (Medio-Cross riboavindextran
solution, 0.1%) were instilled topically on the cornea
every 2 min for a period of 30 min. The cornea was
then illuminated using a Phoenix UV-A system
(Peschke
Meditrade
GmbH,
Huenenberg,
Switzerland), UVA 365 nm, with an irradiance of
3 mW/cm2 and a total dose of 5.4 J/cm2 over 30 min.
During the period of UV illumination, riboavin was
administered to the eye every 2 min. Patients were
continued with the same topical medications that
Shetty R, et al. Br J Ophthalmol 2014;98:10331035. doi:10.1136/bjophthalmol-2014-304944
1033
Downloaded from http://bjo.bmj.com/ on November 26, 2014 - Published by group.bmj.com
Clinical science
were being used prior to CXL. Topical corticosteroids or NSAIDs
were not prescribed after the crosslinking procedure.
RESULTS
In all, 15 eyes of 15 patients including 10 men and ve women
with culture proven non-healing microbial keratitis were
included in the study. Mean age of the patients was 51
13.38 years (range 2771 years). Based on the smear and
culture reports, nine patients had bacterial keratitis and six had
fungal keratitis. The most common bacteria isolated were
staphylococci and aspergillus was the most common fungus.
Seven patients had hypopyon at the time of presentation.
Table 1 gives the pre-CXL and post-CXL details of all patients.
All patients who underwent CXL had resolution of pain on
the rst postoperative day. In four patients with hypopyon
cornea ulcer, there was an increase in hypopyon by the third
postoperative day. There was an appearance of hypopyon in
three patients who did not have hypopyon prior to CXL
(gures 14). In patients who responded to CXL (nine out of
15), the mean time for epithelial healing was 21.36.14 days
and the mean time for resolution of corneal inltrate was 33.44
6.2 days. Of the seven patients who either had an increase or
appearance of hypopyon, three patients underwent therapeutic
keratoplasty while in the other four, the resolution of hypopyon
took longer than the resolution of the corneal inltrate.
The mean preoperative score on the Wong-Baker FACES Pain
Rating Scale was 8.270.73 and the mean postoperative score was
0.530.85 indicating that there was a signicant reduction in pain.
No intraoperative complications were noted.
DISCUSSION
In patients undergoing therapeutic keratoplasty for non-healing
microbial keratitis, approximately a third of transplanted grafts
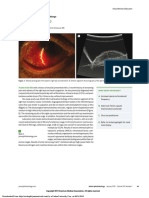
Figure 1 Preoperative non-resolving bacterial keratitis with anterior
stromal inltrate and hypopyon.
become re-infected.12 There has therefore been a constant quest
to nd an alternative to therapeutic keratoplasty when medical
management fails.
Tsugita et al13 showed that the combination of riboavin and
UVA caused a deactivation of the RNA in tobacco mosaic virus.
Martins et al opined that a combination of UVAriboavin has
antibacterial properties in vitro against microorganisms causing
microbial keratitis.9 Hence, we evaluated the effectiveness of
CXL in our patients with infective keratitis. We found that in
patients with supercial corneal inltrates involving only the
anterior third or less of the stroma, there was a better response
than in those cases with deeper inltrates.
According to previous studies, the treatment seems to be most
effective in blocking corneal melt caused by Gram-negative bacteria (92%) followed by Gram-positive bacteria (84%), acanthamoeba (71%) and nally fungi (61%).1420 In our experience,
bacterial keratitis has a better prognosis compared with fungal
Table 1 Details of patients with non-resolving microbial keratitis showing both precollagen and postcollagen crosslinking parameters
Age/
gender
Clinical
diagnosis
Microbiology
reports
Depth of
infiltrate
36/M
42/M
G +ve
G ve
Staph.
Pseudomonas
68/F
52/M
47/M
65/M
G
G
G
G
Staph.
Strepto.
Staph.
Pseudomonas
Superficial stroma
Full thickness ring
infiltrate
Surface infiltrate
Full thickness
Superficial stromal
Anterior stroma
71/F
G +ve
Staph.
36/M
G ve
Inconclusive
53/M
27/F
G +ve
Fungal
Staph.
Aspergillus
58/M
Fungal
Candida
65/F
Fungal
Fusarium
43/M
Fungal
54/F
48/M
Fungal
Fungal
+ve
+ve
+ve
ve
Anterior third of
stroma
Full thickness
Hypopyon
Post-CXL response
No
5 mm
Healed with scar
Non-resolving;
increase in hypopyon
Healed with scar
Non-resolving
Healed with scar
Healed with scar;
hypopyon
Healed with scar
No
4 mm
No
No
No
3 mm
Superficial stromal
Anterior third of
stroma
Deep stromal and
endothelial plaque
Superficial +
mid-deep stroma
No
5 mm
Aspergillus
Anterior stroma
1 mm
Candida
Aspergillus
Deep stroma
Anterior third
stroma
2 mm
No
2 mm
No
Non-resolving;
increase in hypopyon
Healed with scar
Healed with scar
Increase in hypopyon
Non-resolving
Partial scar;
non-resolving;
hypopyon
Healed with scar;
increase in hypopyon
Non-resolving
Healed with scar;
hypopyon
Time for
epithelial
healing
Time for resolution
of infiltrate
Time for
resolution of
hypopyon
14 days
4 weeks
No hypopyon
Non-resolving
18 days
15 days
28 days
4 weeks
4 weeks
5 weeks
No hypopyon
Non-resolving
No hypopyon
7 weeks
21 days
5 weeks
Non-resolving
14 days
26 days
4 weeks
6 weeks
No hypopyon
8 weeks
Non-resolving
Non-resolving
28 days
Only the superficial
infiltrate resolved in
5 weeks
6 weeks
8 weeks
28 days
5 weeks
Non-resolving
6 weeks
G +ve- Gram positive; G -ve- Gram negative; Staph.- Staphylococci species; Strepto.- Streptococci species.
1034
Shetty R, et al. Br J Ophthalmol 2014;98:10331035. doi:10.1136/bjophthalmol-2014-304944
Downloaded from http://bjo.bmj.com/ on November 26, 2014 - Published by group.bmj.com
Clinical science
Figure 4 Post-CXL at 7 weeks showing complete resolution of
corneal inltrate with appearance of hypopyon.
Figure 2 Post-CXL at 8 weeks showing complete resolution of
corneal inltrate with persisting hypopyon.
keratitis probably because of the fact that most of the bacterial
keratitis involved only the supercial part of the corneal stroma.
We also noticed that all patients who underwent CXL had
resolution of pain on the rst postoperative day. The possible
explanation for this could be damage to the subepithelial nerve
plexus by the riboavinUVA combination due to chemical
denervation. The reduction of corneal sensation in all patients
post-CXL supports this hypothesis.
The other important nding was that there was an increase in
hypopyon in four patients post-CXL and appearance of hypopyon in three patients. We attribute this increase or appearance of
hypopyon possibly due to the penetration of riboavin through
the inamed and oedematous stroma into an already inamed
anterior chamber causing further inammation. It was also
noted that the hypopyon took a longer time to resolve than the
re-epithelisation and resolution of surface inltrate.
The main drawback of the study was that it was not known if
the cases of microbial keratitis would have responded to topical
medications if they were continued for a longer period of time;
however, CXL did accelerate healing once it was performed.
In conclusion, CXL appears to be an effective procedure in
treating non-resolving microbial keratitis with supercial stromal
involvement. CXL can be an effective adjunctive treatment and
add to the armamentarium of treatment modalities in the management of resistant microbial keratitis. However, further
studies are required to streamline the indications, protocol and
safety prole of CXL in the management of microbial keratitis.
Contributors All authors have contributed in the preparation of the manuscript
and the clinical study.
Competing interests None.
Ethics approval Narayana Nethralaya Ethics Committee.
Provenance and peer review Not commissioned; externally peer reviewed.
REFERENCES
1
2
3
4
5
6
7
8
9
10
11
12
13
14
15
16
17
18
19
Figure 3 Non-resolving fungal keratitis after 2 weeks of treatment
with topical antifungals.
20
Shetty R, et al. Br J Ophthalmol 2014;98:10331035. doi:10.1136/bjophthalmol-2014-304944
Whitcher JP, Srinivasan M, Upadhyay MP. Corneal blindness: a global perspective.
Bull World Health Organ 2001;79:21421.
Burd EM, Ogawa GSH, Hyndiuk RA. Bacterial keratitis and conjunctivitis. In:
Smolin G, Thoft RA, eds. The cornea scientic foundations and clinical practice. 3rd
edn. Boston: Little, Brown, & Co, 1994:11567.
Keay L, Edwards K, Naduvilath T, et al. Microbial keratitis predisposing factors and
morbidity. Ophthalmology 2006;113:10916.
Wong T, Ormonde S, Gamble G, et al. Severe infective keratitis leading to hospital
admission in New Zealand. Br J Ophthalmol 2003;87:11038.
Jones DB. Decision-making in the management of microbial keratitis.
Ophthalmology 1981;88:81420.
BertinoJ S. Impact of antibiotic resistance in the management of ocular infections:
the role of current and future antibiotics. ClinOphthalmol 2009;3:50721.
Goodrich RP. The use of riboavin for inactivation of pathogens in blood products.
Vox Sang 2000;78:21115.
McAteer MJ, Tay-Goodrich B, Doane S. Photoinactivation of virus in packed red
blood cell units using riboavin and visible light. Transfusion 2000;3(Suppl):99S.
Martins SA, Combs JC, Noguera G, et al. Antimicrobial efcacy of riboavin/UVA
combination (365 nm) in vitro for bacterial and fungal isolates: a potential new
treatment for infectious keratitis. Invest Ophthalmol Vis Sci 2008;49:34028.
Schrier A, Greebel G, Attia H, et al. In vitro antimicrobial efcacy of riboavin and
ultraviolet light on Staphylococcus aureus, methicillin-resistant Staphylococcus
aureus, and Pseudomonas aeruginosa. J Refract Surg 2009;25:S799802.
Makdoumi K, Backman A, Mortensen J, et al. Evaluation of antibacterial efcacy of
photo-activated riboavin using ultraviolet light (UVA). Graefes Arch Clin Exp
Ophthalmol 2010;248:20712.
Shi W, Liu M, Gao H, et al. Perioperative treatment and prognostic factors for
penetrating keratoplasty in Acanthamoeba keratitis unresponsive to medical
treatment. Graefes Arch Clin Exp Ophthalmol 2009;247:13838.
Tsugita A, Okada Y, Uchara K. Photosensitized inactivation of ribonucleic acids in
the presence of riboavin. Biochim Biophys Acta 1965;103:3603.
Anwar HM, El-Danasoury AM, Hashem AN. Corneal collagen crosslinking in the
treatment of infectious keratitis. Clin Ophthalmol 2011;5:127780.
Makdoumi K, Mortensen J, Crafoord S. Infectious keratitis treated with corneal
crosslinking. Cornea 2010;29:13538.
Morn H, Malmsj M, Mortensen J, et al. Riboavin and ultraviolet a collagen
crosslinking of the cornea for the treatment of keratitis. Cornea 2010;29:1024.
Iseli HP, Thiel MA, Hafezi F, et al. Ultraviolet A/riboavin corneal cross-linking
for infectious keratitis associated with corneal melts. Cornea 2008;27:5904.
Khan YA, Kashiwabuchi RT, Martins SA, et al. Riboavin and ultraviolet light a
therapy as an adjuvant treatment for medically refractive Acanthamoeba keratitis:
report of 3 cases. Ophthalmology 2011;118:32431.
Martins SA, Combs JC, Noguera G, et al. Antimicrobial efcacy of riboavin/UVA
combination (365 nm) in vitro for bacterial and fungal isolates: a potential new
treatment for infectious keratitis. Invest Ophthalmol Vis Sci 2008;49:34028.
Price MO, Tenkman LR, Schrier A, et al. Photoactivated riboavin treatment of infectious
keratitis using collagen cross-linking technology. J Refract Surg 2012;28:70613.
1035
Downloaded from http://bjo.bmj.com/ on November 26, 2014 - Published by group.bmj.com
Collagen crosslinking in the management of
advanced non-resolving microbial keratitis
Rohit Shetty, Harsha Nagaraja, Chaitra Jayadev, Yathish Shivanna and
Thungappa Kugar
Br J Ophthalmol 2014 98: 1033-1035 originally published online April 7,
2014
doi: 10.1136/bjophthalmol-2014-304944
Updated information and services can be found at:
http://bjo.bmj.com/content/98/8/1033
These include:
References
Email alerting
service
Topic
Collections
This article cites 18 articles, 3 of which you can access for free at:
http://bjo.bmj.com/content/98/8/1033#BIBL
Receive free email alerts when new articles cite this article. Sign up in the
box at the top right corner of the online article.
Articles on similar topics can be found in the following collections
Cornea (464)
Ocular surface (553)
Eye (globe) (632)
Neurology (1220)
Notes
To request permissions go to:
http://group.bmj.com/group/rights-licensing/permissions
To order reprints go to:
http://journals.bmj.com/cgi/reprintform
To subscribe to BMJ go to:
http://group.bmj.com/subscribe/
You might also like
- MOA Template - Ambulance TemplateDocument4 pagesMOA Template - Ambulance TemplatevgruayaNo ratings yet
- USMLE Step 3 Lecture Notes 2021-2022: Pediatrics, Obstetrics/Gynecology, Surgery, Epidemiology/Biostatistics, Patient SafetyFrom EverandUSMLE Step 3 Lecture Notes 2021-2022: Pediatrics, Obstetrics/Gynecology, Surgery, Epidemiology/Biostatistics, Patient SafetyRating: 5 out of 5 stars5/5 (2)
- Handbook of Consumer Finance Research - 2sd Edition PDFDocument382 pagesHandbook of Consumer Finance Research - 2sd Edition PDFLuiz AlvesNo ratings yet
- Manage WSH Risks in Construction Industries - Courseware Learner's Guide V2 0Document378 pagesManage WSH Risks in Construction Industries - Courseware Learner's Guide V2 0Angie Ee50% (2)
- School of Graduate Studies KNUSTDocument32 pagesSchool of Graduate Studies KNUSTKwajo Asante100% (5)
- BR J Ophthalmol 1999 Das 1050 5Document7 pagesBR J Ophthalmol 1999 Das 1050 5xoxotheNo ratings yet
- Penetrating Keratoplasty in Active Acanthamoeba KeratitisDocument5 pagesPenetrating Keratoplasty in Active Acanthamoeba Keratitisdrvishalkulkarni2007No ratings yet
- Review Article: Profile of Corneal Ulcer in A Tertiary Eye Care CentreDocument6 pagesReview Article: Profile of Corneal Ulcer in A Tertiary Eye Care CentreNadhila ByantNo ratings yet
- Jurnal Mata 1Document9 pagesJurnal Mata 1marhayudi15No ratings yet
- Comparative Study On The Efficacy of Non-Steroidal, Steroid and Non-Use Anti Inflammatory in The Treatment of Epidemic ConjungtivitisDocument6 pagesComparative Study On The Efficacy of Non-Steroidal, Steroid and Non-Use Anti Inflammatory in The Treatment of Epidemic ConjungtivitisVisakha VidyadeviNo ratings yet
- Prajna2019 PDFDocument24 pagesPrajna2019 PDFJennifer ChávezNo ratings yet
- CorinebakteriumDocument6 pagesCorinebakteriummillaNo ratings yet
- AgashemicrosporidiaDocument5 pagesAgashemicrosporidiargroup331No ratings yet
- Posted at The Institutional Resources For Unique Collection and Academic Archives at Tokyo Dental College, Available From Http://ir - Tdc.ac - JPDocument20 pagesPosted at The Institutional Resources For Unique Collection and Academic Archives at Tokyo Dental College, Available From Http://ir - Tdc.ac - JPwhiezardNo ratings yet
- Bacterial KeratitisDocument6 pagesBacterial KeratitisMelia RahmayantiNo ratings yet
- Microbiological Profile and Antimicrobial Sensitivity Pattern of Culture Positive Bacterial Keratitis: A Prospective Observational StudyDocument5 pagesMicrobiological Profile and Antimicrobial Sensitivity Pattern of Culture Positive Bacterial Keratitis: A Prospective Observational StudyBombong NurpaginoNo ratings yet
- TranslateDocument5 pagesTranslatenoviadewaniNo ratings yet
- Fungal Keratitis and Ocular Surface Squamous Neoplasia in A HIV Positive PatientDocument4 pagesFungal Keratitis and Ocular Surface Squamous Neoplasia in A HIV Positive PatientSherly AsrianiNo ratings yet
- Diagnosis and Management of Microbial Keratitis: AIOS Guidelines ForDocument24 pagesDiagnosis and Management of Microbial Keratitis: AIOS Guidelines ForKukuh Rizwido PrasetyoNo ratings yet
- Ojsadmin, 5-1Document5 pagesOjsadmin, 5-1Abeer AlrofaeyNo ratings yet
- Jurnal MataDocument28 pagesJurnal MatamarinatamiNo ratings yet
- 005 PDFDocument7 pages005 PDFNely KartikaNo ratings yet
- Presumed TB Choroiditis 2015Document3 pagesPresumed TB Choroiditis 2015TrinitaNo ratings yet
- Bak TeriDocument4 pagesBak TeriHawania IINo ratings yet
- Risk Factors and Clinical Outcomes of Bacterial AnDocument9 pagesRisk Factors and Clinical Outcomes of Bacterial AnAgus VirdianNo ratings yet
- Mucormycosis The Deadly Fungus A Case Report.50Document5 pagesMucormycosis The Deadly Fungus A Case Report.50rinakartikaNo ratings yet
- Corticosteroids For Bacterial Keratitis - The Steroids For Corneal Ulcers Trial (SCUT)Document8 pagesCorticosteroids For Bacterial Keratitis - The Steroids For Corneal Ulcers Trial (SCUT)Bela Bagus SetiawanNo ratings yet
- Clinical Study: Effects of Lamellar Keratectomy and Intrastromal Injection of 0.2% Fluconazole On Fungal KeratitisDocument11 pagesClinical Study: Effects of Lamellar Keratectomy and Intrastromal Injection of 0.2% Fluconazole On Fungal Keratitis何燕No ratings yet
- Amniotic Membrane Transplantation Combined With Antiviral and Steroid Therapy For Herpes Necrotizing Stromal KeratitisDocument7 pagesAmniotic Membrane Transplantation Combined With Antiviral and Steroid Therapy For Herpes Necrotizing Stromal KeratitisnelyNo ratings yet
- Oftalmologi 3Document3 pagesOftalmologi 3Jericho JeruzalemNo ratings yet
- Jceh 12 30 021Document3 pagesJceh 12 30 021Tatik HandayaniNo ratings yet
- InfectiouskeratitisDocument9 pagesInfectiouskeratitisJampala SrinivasNo ratings yet
- Jurnal Mata 2Document5 pagesJurnal Mata 2lathifa_nurNo ratings yet
- Treatment Ineffective Hydroxychloroquine PDFDocument4 pagesTreatment Ineffective Hydroxychloroquine PDFMaria Alejandra' LopezNo ratings yet
- Etm 11 06 2391Document4 pagesEtm 11 06 2391noor hidayahNo ratings yet
- Corneal UlcerDocument6 pagesCorneal UlcerChanifah SitiNo ratings yet
- Journal of KeratitisDocument16 pagesJournal of KeratitisAan AchmadNo ratings yet
- Document PDFDocument9 pagesDocument PDFNur Akbar MangindaraNo ratings yet
- Antimicrobial Effect of Platelet-Rich Plasma AgainDocument6 pagesAntimicrobial Effect of Platelet-Rich Plasma AgainPhong TruongNo ratings yet
- A Painful Red EyeDocument2 pagesA Painful Red EyeCristhian Agustin ParedesNo ratings yet
- Empirictx NTMDocument9 pagesEmpirictx NTMluck2livNo ratings yet
- New Protocol To Treat Corneal Ulcer: 2 Years Retrospective ExperienceDocument4 pagesNew Protocol To Treat Corneal Ulcer: 2 Years Retrospective Experiencetocx1xNo ratings yet
- Clinical Presentation and Microbial Analyses of Contact Lens Keratitis An Epidemiologic StudyDocument4 pagesClinical Presentation and Microbial Analyses of Contact Lens Keratitis An Epidemiologic StudyFi NoNo ratings yet
- Schechter 2015Document8 pagesSchechter 2015joseph rivaldoNo ratings yet
- Clinical Study: Outcome and Prognostic Factors For Traumatic Endophthalmitis Over A 5-Year PeriodDocument8 pagesClinical Study: Outcome and Prognostic Factors For Traumatic Endophthalmitis Over A 5-Year PeriodannisaNo ratings yet
- Tinea Corporis Caused by Microsporum Audouinii: Case ReportDocument5 pagesTinea Corporis Caused by Microsporum Audouinii: Case ReportArasti Qisthi VanzifaNo ratings yet
- Long-Term Outcomes of Pediatric Penetrating Keratoplasty For Herpes Simplex Virus KeratitisDocument6 pagesLong-Term Outcomes of Pediatric Penetrating Keratoplasty For Herpes Simplex Virus KeratitisgallaNo ratings yet
- Contact Lens & Anterior EyeDocument4 pagesContact Lens & Anterior Eyedori45No ratings yet
- 2016 Article 294 PDFDocument7 pages2016 Article 294 PDFChato Haviz DanayomiNo ratings yet
- Endophthalmitis Patients Seen in A Tertiary Eye Care Centre in Odisha: A Clinico-Microbiological AnalysisDocument8 pagesEndophthalmitis Patients Seen in A Tertiary Eye Care Centre in Odisha: A Clinico-Microbiological AnalysisSurendar KesavanNo ratings yet
- Conjunctivitis As A Manifestation of Wegener 'S GranulomatosisDocument5 pagesConjunctivitis As A Manifestation of Wegener 'S GranulomatosisAsd DsaNo ratings yet
- Prevalence and Prognosis of Corneal Perforation Patient in Beijing ChinaDocument4 pagesPrevalence and Prognosis of Corneal Perforation Patient in Beijing Chinaalifah syarafinaNo ratings yet
- 9 Samuel EtalDocument4 pages9 Samuel EtaleditorijmrhsNo ratings yet
- Phacoemulsification Versus Manual Small Incision Cataract Surgery in Patients With Fuchs Heterochromic IridocyclitisDocument5 pagesPhacoemulsification Versus Manual Small Incision Cataract Surgery in Patients With Fuchs Heterochromic IridocyclitisMichael Christopher KadangNo ratings yet
- Jurnal Mata 5 KEVIN PDFDocument10 pagesJurnal Mata 5 KEVIN PDFKevinNo ratings yet
- Hydroxypropyl Cellulose Ophthalmic Inserts (Lacrisert) Reduce The Signs and Symptoms of Dry Eye Syndrome and Improve Patient Quality of LifeDocument9 pagesHydroxypropyl Cellulose Ophthalmic Inserts (Lacrisert) Reduce The Signs and Symptoms of Dry Eye Syndrome and Improve Patient Quality of LifekikinantiNo ratings yet
- Admin, 24 Mukundh Chaithanya FINALDocument5 pagesAdmin, 24 Mukundh Chaithanya FINALLaili Nurul IslamiNo ratings yet
- JurnalMata Pigrum Keratitis 1471-2415!13!31Document4 pagesJurnalMata Pigrum Keratitis 1471-2415!13!31Alfrino Patriando AdamNo ratings yet
- Treatment of Vitiligo With Narrow-Band UVB and Topical Gel Containing Catalase and Superoxide DismutaseDocument5 pagesTreatment of Vitiligo With Narrow-Band UVB and Topical Gel Containing Catalase and Superoxide DismutaseBen IntosiusNo ratings yet
- Zoster Sine HerpeteDocument7 pagesZoster Sine HerpeteLalo RCNo ratings yet
- Efficacy and Safety of Subconjunctival Bevacizumab For Recurrent PterygiumDocument4 pagesEfficacy and Safety of Subconjunctival Bevacizumab For Recurrent PterygiummayangestowoNo ratings yet
- Assessment and Management of Patient's With Allergic ReactionsDocument13 pagesAssessment and Management of Patient's With Allergic ReactionsLau ColastreNo ratings yet
- Infant Transport Incubator: Isolette® Ti500Document4 pagesInfant Transport Incubator: Isolette® Ti500Suyatno HendroNo ratings yet
- Informed Consent TimetableDocument11 pagesInformed Consent TimetableAkita C.No ratings yet
- German Atv Rules and Standards: Atv Standard ATV-A 106EDocument29 pagesGerman Atv Rules and Standards: Atv Standard ATV-A 106EMehmet Emre BastopcuNo ratings yet
- PHEngg Handouts and Workbook 4Document175 pagesPHEngg Handouts and Workbook 4AMmarNo ratings yet
- Nursing Seminar 1 SAS Session 17Document8 pagesNursing Seminar 1 SAS Session 17ZiaNo ratings yet
- IS 13115 (B) (1991) - Portable First Aid Kit For General Use (Bi-Lingual)Document10 pagesIS 13115 (B) (1991) - Portable First Aid Kit For General Use (Bi-Lingual)navitaNo ratings yet
- Professional Writing The Dangers of CrammingDocument2 pagesProfessional Writing The Dangers of Crammingadhiimull gantengNo ratings yet
- MetforminDocument14 pagesMetforminRoberto AlexiNo ratings yet
- Dogs As Human Companions: A Review of The Relationship: January 1995Document28 pagesDogs As Human Companions: A Review of The Relationship: January 1995Vladut BratfaleanNo ratings yet
- Northern NVProvider DirectoryDocument11,316 pagesNorthern NVProvider DirectorymedobrundoNo ratings yet
- Fifty Most Cited Research Papers in Child PornograDocument7 pagesFifty Most Cited Research Papers in Child PornograKush TiwariNo ratings yet
- Research Material PDFDocument125 pagesResearch Material PDFNikita NelsonNo ratings yet
- 9 Golden Rule in RefineryDocument3 pages9 Golden Rule in RefineryXuân HòaNo ratings yet
- Leukemia PowerpointDocument11 pagesLeukemia Powerpointapi-281804167No ratings yet
- RFQ-97 For Supply of Biscuit & Soap-2Document1 pageRFQ-97 For Supply of Biscuit & Soap-2Prodip Debnath NayanNo ratings yet
- Standards: Overview of The StandardsDocument5 pagesStandards: Overview of The StandardsAlice Lara PalicpicNo ratings yet
- HistoryDocument3 pagesHistoryDammika Madhusankha100% (1)
- Singlife Cancer Cover Plus BrochureDocument10 pagesSinglife Cancer Cover Plus BrochureTulip TyNo ratings yet
- Annotated Bibliography APA Working TitleDocument5 pagesAnnotated Bibliography APA Working Titleapi-357824256No ratings yet
- RHS 2019-20Document262 pagesRHS 2019-20Teja naveenNo ratings yet
- Alltech Poultry Droppings PosterDocument1 pageAlltech Poultry Droppings PosterAndrew JabakumarNo ratings yet
- 5014-Prescription Regulation TableDocument2 pages5014-Prescription Regulation TableUrugonda VenumadhavNo ratings yet
- AQA Unit 2 Sociology of Health (5) Disability: The Biomedical Approach To DisabilityDocument10 pagesAQA Unit 2 Sociology of Health (5) Disability: The Biomedical Approach To DisabilityClean ToneNo ratings yet
- Reliance HealthGain Policy - Brochure PDFDocument2 pagesReliance HealthGain Policy - Brochure PDFPranavH RigvediNo ratings yet
- Monthly Service Delivery Report: Health Management Information SystemDocument2 pagesMonthly Service Delivery Report: Health Management Information SystemPrakash MahajanNo ratings yet