Chest Discomforts.pptx
- 1. CHEST DISCOMFORTS (PAIN) MUKESH SUNDARARAJAN
- 2. Learning Outcome DEFINITION TYPE OF CHEST PAIN ETIOLOGY CHARACTERISTIC OF CARDIAC CHEST PAIN ISCHAEMIC CARDIAC PAIN VS NON- CARDIAC CHEST PAIN DIFFERENTIAL DIAGNOSIS
- 3. Chest Pain Definition: • A general term for any dull, aching pain in the thorax. It can be cardiac or non-cardiac related.
- 4. ETIOLOGY Cardiac • Myocardial ischemia & trauma • Angina pectoris • Acute Coronary Syndromes Non-Cardiac • Aortic stenosis • Aortic dissection • Pericarditis • Pulmonary embolism • Pulmonary hypertension • Pneumonia/pleuritis • Spontaneoushypertension • Esophageal reflux • Esophageal spasm • Peptic ulcer • Gallbladder disease • Musculoskeletal disease • Herpes zoster •Emotional & psychiatric conditions
- 5. Types Of Chest Pain Pleuritic Sharp Burning Pressure Tightness Heaviness Burning Tearing/ripping Burning Pressure Angina, unstable angina, acute MI Pericarditis Aortic dissection Gallbladder disease Pul. Embolism, Pneumonia, Pleuritis, Spontaneous hypertension Esophageal reflux, peptic ulcer, herpes zoster Pressure Tightness Burning Variable Aching Emotional & psychiatric conditions Esophageal spasm Musculoskeletal disease
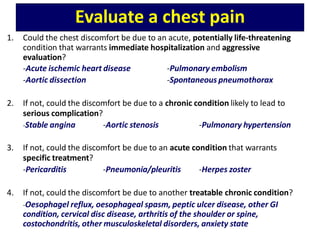
- 6. Evaluate a chest pain 1. Could the chest discomfort be due to an acute, potentially life-threatening condition that warrants immediate hospitalization and aggressive evaluation? -Acute ischemic heart disease -Aortic dissection -Pulmonary embolism -Spontaneous pneumothorax 2. If not, could the discomfort be due to a chronic condition likely to lead to serious complication? -Stable angina -Aortic stenosis -Pulmonary hypertension 3. If not, could the discomfort be due to an acute condition that warrants specific treatment? -Pericarditis -Pneumonia/pleuritis -Herpes zoster 4. If not, could the discomfort be due to another treatable chronic condition? -Oesophagel reflux, oesophageal spasm, peptic ulcer disease, other GI condition, cervical disc disease, arthritis of the shoulder or spine, costochondritis, other musculoskeletal disorders, anxiety state
- 7. Initial Evaluation of Suspected Cardiac Pain Importance of initial evaluation:- • Crucial process • Determine the:- – Nature and extent of any underlying heart disease – Risk of serious adverse event – Management
- 8. Characteristics of ISCHAEMIC cardiac Pain • Characteristic of pain • Site • Radiation • Provocation • Onset • Associated features
- 9. Character • Dull, constricting, choking or heavy • Squeezing, crushing, burning or aching • Breathlessness • Discomfort > pain
- 10. Site • Centre of the chest • Derivation of the nerve supply to the heart & mediastinum (sensory sympathetic cardiac nerves; T1-T5, mostly dorsal root ganglion Lt.) Radiation • Radiate to neck, jaw & upper or even lower arms • Occasionally, at the sites of radiation or in the back
- 12. Provocation • Angina pain: during exertion and promptly relieved by rest (<5 minutes), pain may exacerbated by emotion but occur more readily by exertion; large meal, cold wind • Crescendo/Unstable angina: similar pain can be precipitated by minimal exertion or at rest • Decubitus angina: increase venous return/preload by lying down can provoke pain in vulnerable patients
- 13. Onset • Myocardial infarction (MI): Pain of MI takes several minutes or longer to develop • Angina: Pain builds up gradually in proportion to the intensity of exertion • Aortic dissection, massive pulmonary embolism or pneumothorax : Pain is very sudden or instantaneous • Musculoskeletal or psychological: Pain occur after exertion
- 14. Associated features • Autonomic disturbance; sweating, nausea, vomiting • Breathlessness: pulmonary congestion from transient ischaemic Lt. ventricular dysfunction
- 15. CHARACTERISTIC ISCHAEMIC CARDIAC CHEST PAIN NON-CARDIAC CHEST PAIN LOCATION Central, diffuse Peripheral, localised RADIATION Jaw/neck/shoulder/arm (occasionally back) Other or no radiation CHARACTER Tight, squeezing, choking Sharp, stabbing, catching PRECIPITATION Exertion and/or emotion Spontaneous, provoked by posture,respiration or palpitation RELIEVING FACTOR Rest, quick response to nitrates Not relieved by rest, slow or no response to nitrates ASSOCIATED FEATURES Breathlessness Respiratory, gastrointestinal, locomotor or psychological
- 16. Differential Diagnosis of Chest Pain • Anxiety/emotion • Cardiac • Aortic • Oesophageal • Lungs/pleura • Musculoskeletal • Neurological
- 17. Anxiety • Common cause for atypical chest pain • Lack of relationship with exercise • Receiving bad news Cardiac • Myocardial ishaemia (angina), MI, myocarditis, pericarditis, mitral valve prolapse • Myocarditis & pericarditis: – Pain felt retrosternally, to the Lt. of the sternum, or in the Lt./Rt. Shoulder – Intensity varies with movement and phase of respiration. ‘sharp’ and may ‘catch’ during inspiration, coughing or lying flat. – Occasionally, history of prodromal viral illness
- 18. Aortic • Aortic dissection, aortic aneurysm • Aortic dissection: – Pain is severe, sharp and tearing – Penetrating through to the back – Abrupt in onset – Pain follows path of the dissection
- 20. Oesophageal • Oesophagitis, oesophageal spasm, Mallory-Weiss syndrome • Pressure, tightness, burning • Retrosternal • Mimic angina very closely – Sometimes precipitated by exercise – Sometimes relieved by nitrates • Elicit history of chest pain to supine posture or eating, drinking or oesophageal reflux • Radiates to the back
- 21. Lungs/Pleura • Bronchospasm, pulmonary infarct, pneumonia, tracheitis, pneumothorax, pulmonary embolism, malignancy, tuberculosis • Bronchospasm: – Reversible airways obstruction (e.g. asthma): exertional chest tightness that is relieved by rest. Difficult to distinguish from ischaemic chest tightness • Pneumonia, pleuritis and pulmonary embolism: – Pleuritic pain (sharp pain when breathing)
- 22. Musculoskeletal • Osteoarthritis, rib fracture/injury, costochondritis (Tietze’s syndrome), intercostal muscle injury, epidemic myalgia (Bornholm disease-by coxsackievirus) • Aching • Very variable in site and intensity • Vary with posture and movement of upper body • Can be accompanied by local tenderness over a rib or costal cartilage • Injuries related to everyday activities or viral infection
- 23. Neurological • Prolapsed intervertebral disc • Herpes zoster (Sharp or burning) • Thoracic outlet syndrome
- 24. Stable Angina VS Acute Coronary Syndrome
- 25. STABLE ANGINA ACUTE CORONARY SYNDROMES (unstable angina, STEMI, NSTEMI) •Effort-related chest or ‘choking in the chest’ •Relationship to physical exertion (and occasionally emotion) of the chest pain •The duration of symptoms should be noted because patients with recent-onset angina are at greater risk • Urgent evaluation •Prolonged, severe cardiac chest pain
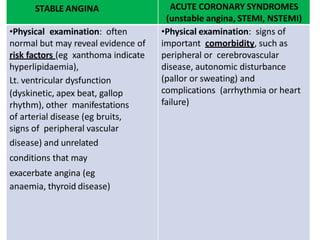
- 26. STABLE ANGINA ACUTE CORONARY SYNDROMES (unstable angina, STEMI, NSTEMI) •Physical examination: often normal but may reveal evidence of risk factors (eg xanthoma indicate hyperlipidaemia), Lt. ventricular dysfunction (dyskinetic, apex beat, gallop rhythm), other manifestations of arterial disease (eg bruits, signs of peripheral vascular disease) and unrelated conditions that may exacerbate angina (eg anaemia, thyroid disease) •Physical examination: signs of important comorbidity, such as peripheral or cerebrovascular disease, autonomic disturbance (pallor or sweating) and complications (arrhythmia or heart failure)
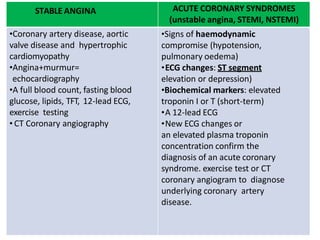
- 27. STABLE ANGINA ACUTE CORONARY SYNDROMES (unstable angina, STEMI, NSTEMI) •Coronary artery disease, aortic valve disease and hypertrophic cardiomyopathy •Angina+murmur= echocardiography •A full blood count, fasting blood glucose, lipids, TFT, 12-lead ECG, exercise testing • CT Coronary angiography •Signs of haemodynamic compromise (hypotension, pulmonary oedema) •ECG changes: ST segment elevation or depression) •Biochemical markers: elevated troponin I or T (short-term) •A 12-lead ECG •New ECG changes or an elevated plasma troponin concentration confirm the diagnosis of an acute coronary syndrome. exercise test or CT coronary angiogram to diagnose underlying coronary artery disease.
- 29. Types Of Chest Pain Pleuritic Sharp Burning Pressure Tightness Heaviness Burning Tearing/ripping Burning Pressure Angina, unstable angina, acute MI Pericarditis Aortic dissection Gallbladder disease Pul. Embolism, Pneumonia, Pleuritis, Spontaneous hypertension Esophageal reflux, peptic ulcer, herpes zoster Pressure Tightness Burning Variable Aching Emotional & psychiatric conditions Esophageal spasm Musculoskeletal disease
- 30. TYPICAL CLINICAL FEATURES OF MAJOR CAUSES OF ACUTE CHEST DISCOMFORT
- 31. Condition Duration Quality Location Associated features Angina 2 min <t< 10 min Pressure, Retrosternal, Precipitated by tightness, often with exertion, heaviness, radiation to or exposure to cold, burning isolated psychologic stress discomfort in neck, jaw, S4 gallop or mitral regurgitation sholders, or murmur during arms- freq. left pain Unstable 10-20 min Similar to Similar to angina Similar to angina angina angina but but occurs with >severe low levels of exertion or even at rest Acute MI Variable; often Similar to Similar to angina Unrelieved with >30 min angina but nitroglycerin >severe May be associated with heart failure or arrhythmia
- 32. Condition Duration Quality Location Associated features Aortic stenosis Recurrent episodes Same as angina Same as angina Late-peaking systolic murmur radiating to carotid arteries Pericarditis Hours-days; may be episodic Sharp Retrosternal or toward cardiac apex; may radiate to Lt. shoulder May be relieved by sitting up and leaning forward Pericardial friction rub Aortic dissection Abrupt onset of unrelenting pain Tearing or ripping sensation ; knifelike Anterior chest offten radiating to back,between shoulder blades Hypertension and/or underlying connective tissue disorder,e.g., Marfan syndrome Pulmonary embolism Abrupt onset; several min- few hours Pleuritic Often lateral, on the side of the embolism Dyspnea, tachypnea, tachycardia and hypotension Pulmonary hypertension Variable Pressure Substernal Dyspnea,signs of increased venous pressure including edema & jv distension
- 33. Condition Duration Quality Location Associated features Pneumonia/ pleuritis Variable Pleuritic Unilateral,often localized Dyspnea, cough, fever, rales, occasional rub Spontaneous hypertension Sudden onset; several hours Pleuritic Lateral to side of pneumothorax Dyspnea, decreased breath sounds on side of pneumothorax Esophageal reflux 10-60 min Burning Substernal, epigastric Worsened by postprandial recumbency Relieved by antacids Esophageal spasm 2-30 min Pressure, tightness, burning Retrosternal Can closely mimic angina Peptic ulcer Prolonged Burning Epigastric, substernal Relieved with food or antacids
- 34. Condition Duration Quality Location Associated features Gallbladder disease Prolonged Burning, pressure Epigastric, Rt. Upper quadrant, substernal May follow meal Musculoskeletal disease Variable Aching Variable Aggravated by movement May be reproduced by localized pressure one examination Herpes zoster Variable Sharp or burning Dermatomal distribution Vesicular rash in area of discomfort Emotional & psychiatric conditions Variable; may be fleeting Variable Variable; may be retrosternal Situational factors may precipitate symptoms Anxiety or depression often detectable with careful history
- 35. Conclusion Topics which are covered:- • Define chest pain • Types of chest pain • Characteristic of cardiac chest pain • Ischaemic cardiac pain vs non-cardiac chest pain • Differential diagnosis
- 36. References • Davidson’s Principles & Practice of Medicine 23rd Edition • Harrison’s Internal Medicine 18th Edition • Hutchinson’s Clinical Method 22nd Edition