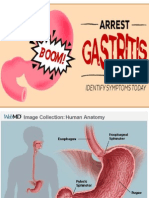
Understanding Gastritis: Causes, Symptoms, and Treatment
Uploaded by
Sania oktaUnderstanding Gastritis: Causes, Symptoms, and Treatment
Uploaded by
Sania oktaCommon questions
Powered by AIAcute gastritis typically has a sudden onset, often caused by stress, chemical irritants like alcohol, or medications that irritate the stomach lining. It is usually temporary and resolves with treatment. Chronic gastritis develops slowly over time and is often attributed to persistent Helicobacter pylori infection, autoimmune responses, or long-term use of non-steroidal anti-inflammatory drugs. Chronic gastritis can lead to more severe long-term effects, such as gastric mucosa metaplasia, increased risk of ulcers, and possibly stomach cancer due to the ongoing inflammation and cellular changes.
Helicobacter pylori contribute to chronic gastritis by infecting the gastric epithelial cells, leading to cell desquamation and a chronic inflammatory response. Physiological changes include glandular destruction and metaplasia, where the body replaces gastric mucosal cells with less elastic desquamosa cells to withstand irritation. Despite providing some resistance to further damage, the reduced elasticity affects peristaltic movement in the stomach, causing pain and contributing to the progression of the condition. Metaplasia and damage from the inflammatory response also lead to blood vessel damage, increasing the risk of bleeding.
Treatment strategies for gastritis include the use of antacids and drugs like proton pump inhibitors and H-2 blockers to reduce stomach acid, avoiding spicy foods, and addressing specific causes. In cases of H. pylori infection, a regimen of antibiotics combined with acid blockers is prescribed. For gastritis caused by pernicious anemia, B-12 vitamin shots are used. Additionally, dietary changes to eliminate irritants such as dairy or gluten may be necessary. These treatments target the underlying issues leading to inflammation and prevent further damage to the stomach lining.
The thinning of the stomach lining in older adults contributes to an increased risk of gastritis because it reduces the natural protective barrier against stomach acid and irritants, making the stomach more susceptible to damage and infection, such as by H. pylori. To prevent gastritis, older adults can avoid excessive use of NSAIDs, maintain a balanced diet, limit alcohol consumption, and manage stress levels. Regular medical check-ups to monitor stomach health and address symptoms early can also be beneficial.
Autoimmune gastritis occurs when the body's immune system attacks cells that constitute the stomach lining, eroding the protective barrier. This attack increases vulnerability to stomach acid, resulting in inflammation. Conditions such as Hashimoto's disease and type 1 diabetes, which involve similar autoimmune responses, heighten the risk. Autoimmune gastritis can also lead to vitamin B-12 deficiency due to impaired absorption in the stomach, further complicating the condition.
Diagnostic methods for confirming gastritis include upper endoscopy, blood tests, and fecal occult blood tests. Upper endoscopy involves inserting a camera-equipped tube to inspect the stomach lining for inflammation, and may include a tissue biopsy. Blood tests can check for anemia, indicating insufficient red blood cells, and screen for H. pylori infection. Fecal occult blood tests check for hidden blood in the stool, a potential sign of gastritis-related bleeding. These tests target symptoms such as abdominal pain, digestive bleeding, and signs of infection.
Lifestyle choices significantly affect gastritis risk, particularly through diet, alcohol consumption, and smoking. High alcohol intake can irritate and erode the stomach lining, increasing risk for acute gastritis, while smoking and an unhealthy diet may exacerbate H. pylori infection or increase its likelihood. Modifying these behaviors, such as reducing alcohol consumption, quitting smoking, and adhering to a balanced diet, can decrease the irritation and inflammation that lead to gastritis, alleviating symptoms and preventing recurrence.
Three risk factors for gastritis include bacterial infection, regular use of pain relievers, and older age. Bacterial infection, particularly with Helicobacter pylori, is a risk factor as it can lead to inflammation of the stomach lining, although not everyone affected develops gastritis due to genetic or lifestyle factors, such as smoking or diet. Regular use of pain relievers like aspirin and ibuprofen decreases a key substance in the stomach lining that protects it from acid. Older age increases risk because the stomach lining tends to thin over time, and the elderly are more prone to H. pylori infection and autoimmune disorders.
Symptoms of gastritis that warrant further diagnostic procedures include a gnawing or burning ache or pain in the upper abdomen, nausea, vomiting, a feeling of fullness after eating, and more severe symptoms like vomiting blood or having black, tarry stools. These symptoms indicate significant inflammation or bleeding, which requires medical investigation such as an endoscopy or blood tests to check for anemia, H. pylori infection, or other serious conditions.
Acute gastritis can be caused by stress, chemical substances such as drugs and alcohol, spicy foods, or acidic food, which lead to irritation of the stomach lining. These substances cause damage by reducing the production of mucus by the epithelial cells that protect the gastric mucosa, making it more vulnerable to digestive juices like hydrochloric acid (HCL). The resulting decrease in mucus protection can cause increased acidity and irritation, leading to symptoms like nausea, vomiting, and anorexia.